Tuesday, June 22, 2010
New Midwifery Association in Rwanda!
The Strengthening Midwifery Symposium had 4 key areas that were addressed: Competency, Education, Regulation and Professional Associations. Prakasamma from India told of the newish Society of Midwives of India (SOMI). It is only 9 years old and they have already had 7 successful conferences. Other areas, such as Nepal and Bhutan, have smaller organizations that are just getting off the ground. In many parts of the world, midwives remain invisible because they do not have professional organizations to represent them. The midwives are "hidden" within the nursing associations. So, we talked about how midwifery globally can be strengthened by the midwives forming their own societies.
My new friend Josephine from Rwanda was inspired. She is from the ministry of health, but she is also a midwife. She told me that after the genocide, they had to start from zero. On our last day there, we were having breakfast and she decided to form the first midwifery association of Rwanda. We actually were trying to decide what it would be called!! It is so inspiring to see women finding their place in the world. I told her that I would be happy to help in whatever way I could.
So today, I received my first email from Rwanda, this is what she said:
"Greetings from Rwanda!
I have passed the message to the midwives I work with, they are very ready to start the midwifery association and move forward."
Wow! Just like that, a midwifery association is born! Congratulations to Josephine and the midwives of Rwanda. I will keep you posted.
Thursday, June 10, 2010
Hope is better than nothing
I keep thinking about Sara from Uganda. She runs a 15-bed clinic along with 2 other midwives. She receives $5 per delivery. Some women come for prenatal care and not too many people come postpartum. Once a healthy baby is born, most of her clients feel they don't need to return.
Sara came all the way to Washington, DC to represent the Ugandan Midwifery Association at the Symposium to Strengthen Midwifery. She received a scholarship to attend Women Deliver. The UMA has over 2000 midwives and was started in 1948 when the government tried to make midwives retire at 55. You can imagine what the midwives said to that! So they formed an organization to better represent themselves to the powers that be. Sara says the UMA is the best midwifery organization in the world.
When the Symposium was almost over, Sara was discouraged and asked me what would happen on the ground. On my last day with Sara, we were walking from store after I had bought chocolate for her to take home to her children. She was hopeful, particularly because I had just made a blog for her that morning. She wants to use the blog to tell the stories of maternal death in Uganda. She wants to post about the midwifery meetings they will have. She has a new vehicle for communication. She is going home with SOMETHING already in her pocket. She says that hope is better than nothing. She says that she has a new friend, she has a blog, and that she knows that she is not forgotten. That the women of Uganda are not forgotten. Sara decided to call her blog, Women for Survival.
I keep thinking about Sara and our fast friendship. I am thinking about our partnership and how one-on-one we can help each other strengthen midwifery. I know so well how the Bay Area's midwifery community has grown simply because of the one-on-one support we give each other. Why can't we do that across the global? I guess I'm saying there's no reason why not.
Sara came all the way to Washington, DC to represent the Ugandan Midwifery Association at the Symposium to Strengthen Midwifery. She received a scholarship to attend Women Deliver. The UMA has over 2000 midwives and was started in 1948 when the government tried to make midwives retire at 55. You can imagine what the midwives said to that! So they formed an organization to better represent themselves to the powers that be. Sara says the UMA is the best midwifery organization in the world.
When the Symposium was almost over, Sara was discouraged and asked me what would happen on the ground. On my last day with Sara, we were walking from store after I had bought chocolate for her to take home to her children. She was hopeful, particularly because I had just made a blog for her that morning. She wants to use the blog to tell the stories of maternal death in Uganda. She wants to post about the midwifery meetings they will have. She has a new vehicle for communication. She is going home with SOMETHING already in her pocket. She says that hope is better than nothing. She says that she has a new friend, she has a blog, and that she knows that she is not forgotten. That the women of Uganda are not forgotten. Sara decided to call her blog, Women for Survival.
I keep thinking about Sara and our fast friendship. I am thinking about our partnership and how one-on-one we can help each other strengthen midwifery. I know so well how the Bay Area's midwifery community has grown simply because of the one-on-one support we give each other. Why can't we do that across the global? I guess I'm saying there's no reason why not.
Monday, June 7, 2010
Call to Action
 Prakasamma from India passing out white ribbons before an introductory ceremony to remember the women who died.
Prakasamma from India passing out white ribbons before an introductory ceremony to remember the women who died.5:05 am
The Call to Action is to strengthen midwifery as a key component to achieving the Millenium Development Goals 4, 5 and 6. These MDGs are the focus of our symposium. In September, 2000, the Millennium Declaration was ratified by 189 heads of state at the United Nations Millennium Summit. This declaration outlined eight broad goals. The Millennium Development Goals (MDGs) represent a global commitment by all nations who signed the Declaration to reduce poverty and improve lives. MDGs 4, 5 and 6 pertain to the health of mothers and children.
MDG 4 is: Reduce by two thirds, between 1990 and 2015, the under-five mortality rate.
MDG 5 is: Reduce by two thirds, between 1990 and 2015, the maternal mortality ratio.
MDG 6 is: Have halted by 2015 and begun to reverse the spread of HIV and AIDS.
The goals are powerful and necessary. The World Health Organization, represented here at the symposium, suggests that we need 334,000 more midwives worldwide in order to meet these goals. The White Ribbon Alliance, that draws attention to maternal mortality globally, states that less than half of the worlds childbearing women are attended by a skilled health worker. Please visit their website, and watch their 2 minute movie about birth and death.
Women Deliver begins today with plenary sessions moderated by Christiane Amanpour and Arriana Huffington. Women Deliver is about empowering women and girls, especially in our poorest countries. Studies show that when women's lives improve, the whole society improves. We can not empower women on this level without talking about reproductive health, safe birthing practices, birth control, and sexual health. Midwifery care has been recognized as part of the process to empower women and achieve the MDG goals.
Gera and I ready to roll.
Sunday, June 6, 2010
Women Deliver
11:19pm
I am finally sitting down at my computer with an Internet connection. Wow. It has been a busy 40 hours of networking, absorbing, thinking, "caring, sharing, and daring," as my new friend, Precious, from the South African Ministry of Health would say. I have been cracked open to the global realities of midwifery. We have been talking about decreasing maternal mortality for 2 days. The exhibit hall for Women Deliver, which will host 3000 people, is booth after booth of international organizations that are working to decrease the number of women DYING in childbirth. DYING. Not infant mortality. Not waterbirth. Not VBACs. WOMEN DYING. IN CHILDBIRTH. This is the issue.
I spoke with a man from Nigeria tonight. Nigeria has the second highest maternal mortality rate in the world. My new friend Josephine, from Rwanda, told me that after the genocide, they had to build midwifery from zero. My friend Sara from Uganda runs a birth clinic where she gets $5 per delivery. My heart is cracked wide to the realities of the world. These brave women who have come SO FAR to tell their stories and seek help from friendly nations. From Chad, Benin, Uganda, South Africa, Nepal, Bhutan, Malawi, Rwanda, Afghanistan, Pakistan, Palestine, India, Uruguay, Chile, Burkina Faso, Sudan. And those are only the ones I am remembering. 40 to 50 countries were represented.
I walked around the exhibit hall and slowly became overwhelmed. Booth after booth told the story of women dying in birth and how each organization was going to tackle the problem. By the time I got through the exhibit hall, I could barely breath. When I sat down, I was crying.
The symposium has been a success on many levels. But Sara from Uganda asks me, what will they do now? What can I expect when I go home? I tell her that tomorrow we will bring that question to the president of the International Confederation of Midwives. I know already in my heart that nothing will change right away. The channels are slow, going through governments and NGOs. The effect "on the ground" will not be felt for perhaps years to come. The Millenium Development Goals are supposed to be reached by 2015. Decreasing maternal mortality by 75%. The pressure is on, and there is hope in the air that much will happen by then.
For now, Sara will go home to her birth clinic-- knowing that she has spoken for the women of Uganda, wondering when change will come.
 New friends from South Africa, Uganda and Rwanda
New friends from South Africa, Uganda and Rwanda
Saturday, June 5, 2010
Symposium on Strengthening Midwifery
6:00 am
Dina and I are here in Washington, DC for the historic event entitled, A Symposium on Strengthening Midwifery. Gera Simkins, MANA president, is still sleeping but Dina and I are going over to the convention center early. Dina will be filming the event. I will be blogging more throughout the day about what this event is all about. Just to give you a taste, last night we had a quick check in with the president of the International Confederation of Midwives, Bridget Lynch. The president of FIGO, the world organization of Obstetricians and Gynecologists was there as well. He's from Egypt. There were also representatives from the United Nations Population Fund and Johns Hopkins. The agenda for today has introductions from the World Health Organization, UNICEF, The World Bank, Johns Hopkins Program for International Education in Gynecology and Obstetrics (JHPIEGO), the Swedish International Development Cooperation Agency (SIDA) and a government perspective from the State Minister of Health from Bangladesh. There will be around 200 people at this event with possible only 3 representatives from the United States' midwifery organizations (us and the ACNM.)
Don't know what to expect fully, but very excited. Stay tuned!
Dina and I are here in Washington, DC for the historic event entitled, A Symposium on Strengthening Midwifery. Gera Simkins, MANA president, is still sleeping but Dina and I are going over to the convention center early. Dina will be filming the event. I will be blogging more throughout the day about what this event is all about. Just to give you a taste, last night we had a quick check in with the president of the International Confederation of Midwives, Bridget Lynch. The president of FIGO, the world organization of Obstetricians and Gynecologists was there as well. He's from Egypt. There were also representatives from the United Nations Population Fund and Johns Hopkins. The agenda for today has introductions from the World Health Organization, UNICEF, The World Bank, Johns Hopkins Program for International Education in Gynecology and Obstetrics (JHPIEGO), the Swedish International Development Cooperation Agency (SIDA) and a government perspective from the State Minister of Health from Bangladesh. There will be around 200 people at this event with possible only 3 representatives from the United States' midwifery organizations (us and the ACNM.)
Don't know what to expect fully, but very excited. Stay tuned!
Friday, May 7, 2010
What You Need to Know About Gestational Diabetes: A Guide for Moms-to-Be
Most Americans know the risks and complications of diabetes and Type 2 diabetes, but gestational diabetes can be an alarming and confusing development for pregnant women. Gestational diabetes is a condition that sometimes occurs in healthy pregnant women who have never had diabetes before but who develop high blood sugar levels when pregnant. The American Diabetes Association estimates that about 135,000 women develop gestational diabetes each year in this country. Women may or may not continue to have diabetes after they give birth, but it is still a serious -- but treatable -- condition that you need to monitor along with your midwife. Here are some facts about gestational diabetes to help you understand the condition -- and how to keep you and your baby healthy -- a little better.
• Gestational diabetes does not cause birth defects: Doctors have found that overweight mothers who had diabetes before becoming pregnant may have increased risk for giving birth to babies with certain defects. Gestational diabetes occurs late in pregnancy, so the risk for birth defects is minimal.
• If left untreated, newborn injury can occur: If mothers do not treat their gestational diabetes, however, their babies may get too big and be injured during birth due to an overworked pancreas and a condition called macrosomia. Another risk is that newborns may have a sudden drop in blood sugar.
• Caused by increased hormone levels: Doctors believe that gestational diabetes is caused by increased levels of hormones like cortisol, estrogen and human placental lactogen. This increase leads to insulin resistance, which means that your pancreas is not able to keep up with the hormones and produce enough insulin to keep your blood sugar in check.
• Know the risk factors: While about half of women who develop gestational diabetes do not have any risk factors, you should be aware of them just in case. They are: becoming obese during pregnancy, having high blood pressure, have a family history of diabetes, are older than 30 years old, or are of a certain ethnicity, like Native American, African, Hispanic or Asian.
• It is treatable: Your midwife will help you come up with the best plan for treating gestational diabetes, from coming up with a weight-loss plan or better nutrition plan, finding ways to get more exercise, and possibly taking insulin injections.
• It may come back in future pregnancies: The American Diabetes Association states that you are two to three times more likely to develop gestational diabetes again during future pregnancies if you have it before. Try to keep your weight in a healthy range and eat nutritious foods to lower your risk of developing Type 2 diabetes.
This guest post is contributed by Jennifer Johnson, who writes on the topics of NP Schools. She welcomes your comments at her email Id: j.johnson19june@gmail.com.
• Gestational diabetes does not cause birth defects: Doctors have found that overweight mothers who had diabetes before becoming pregnant may have increased risk for giving birth to babies with certain defects. Gestational diabetes occurs late in pregnancy, so the risk for birth defects is minimal.
• If left untreated, newborn injury can occur: If mothers do not treat their gestational diabetes, however, their babies may get too big and be injured during birth due to an overworked pancreas and a condition called macrosomia. Another risk is that newborns may have a sudden drop in blood sugar.
• Caused by increased hormone levels: Doctors believe that gestational diabetes is caused by increased levels of hormones like cortisol, estrogen and human placental lactogen. This increase leads to insulin resistance, which means that your pancreas is not able to keep up with the hormones and produce enough insulin to keep your blood sugar in check.
• Know the risk factors: While about half of women who develop gestational diabetes do not have any risk factors, you should be aware of them just in case. They are: becoming obese during pregnancy, having high blood pressure, have a family history of diabetes, are older than 30 years old, or are of a certain ethnicity, like Native American, African, Hispanic or Asian.
• It is treatable: Your midwife will help you come up with the best plan for treating gestational diabetes, from coming up with a weight-loss plan or better nutrition plan, finding ways to get more exercise, and possibly taking insulin injections.
• It may come back in future pregnancies: The American Diabetes Association states that you are two to three times more likely to develop gestational diabetes again during future pregnancies if you have it before. Try to keep your weight in a healthy range and eat nutritious foods to lower your risk of developing Type 2 diabetes.
This guest post is contributed by Jennifer Johnson, who writes on the topics of NP Schools. She welcomes your comments at her email Id: j.johnson19june@gmail.com.
Tuesday, May 4, 2010
EMT Class!
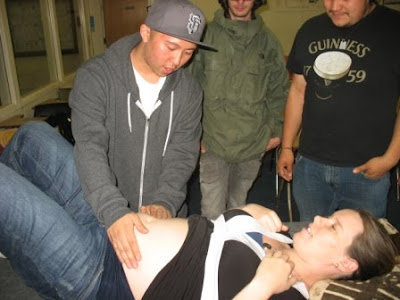
We had a rockin' EMT class today where John the teacher finally let me pay off the bribe I used to let me in the class - I said I would teach the class on birth!! (Did I tell you I'm taking an EMT class so that I can be more prepared to go to Haiti in August? Well, yeah, that's what's going on!) We had live models (thank you Francine, Michelle and Cati), real placentas, Noa Was Born and so much more! How do you possible tell the story of birth from what is an umbilical cord to major complications in 2 hours or less? Anyway, I had a ball and I think most of the class liked it too. Here's the pics:










Monday, April 5, 2010
Two Birth Stories for the Price of One

As soon as I was pregnant with our first child in 2007, I knew I wanted to deliver at home. However, my desire was driven by fear of the hospital rather than love of home birth. To be clear, I am not generally afraid of hospitals or medical procedures, but harbor a strong belief that obstetric care in the US is wildly misguided. I had amassed a binder full of articles pulled from PubMed, read and hi-lighted, and was thoroughly convinced that I was making this decision based on fact and reason, not passion. The thought of checking myself into a L&D ward during a perfectly normal labor brought me to tears, with visions of well-intentioned routine precautions derailing my labor. To be sure, it was a months-long struggle gaining the support of my husband. He was convinced that the articles published to date were not statistically significant, and did not understand how a woman's confidence in herself and her environment could affect the odds of success. Finally, after seeing The Business of Being Born (and me in tears yet again), my husband acquiesced. A short documentary did for me what months of debate based on published medical literature could not. God bless Rikki Lake.
Coming into the BAHC community from this self-described rational perspective, there were many aspects of the midwife style of care which we found strange and confusing. To start, my husband and I hardly knew what to do with our hour-long prenatal care visits with Maria. We would talk about this afterwards, wondering why we had to set aside so much time out of our busy schedules (let alone Maria's) for these appointments, which sometimes seemed to have more silent pauses than agenda items. I found it odd that Maria would palpate my abdomen and talk to me about the indicators of where the baby was; no OB had ever really touched anything except my vagina or breasts. I listened with some skepticism as Maria coached me through how to protect and nurture my belly and the baby through the second and third trimester, and postures which could encourage the baby to turn to a favorable position. By contrast, nothing of this sort was addressed by the OB providers whom I was seeing for concurrent care. Anand and I both rolled our eyes walking into Scarlet Sage to buy herbal supplements at 36 weeks, until I felt the wonderful practice contractions brought on by whatever tincture Maria had recommended. Because we were blessed with an uneventful pregnancy, we had no need to test the limits of Maria's knowledge further; in retrospect, I know we would not have been disappointed.
Compared to other birth stories shared here, Rohan's birth was somewhat mundane. But to me, this average textbook birth was beautiful and perfect. We cherish every memory of that day, frequently reminisce together, and are eager to regale any willing friends with the story. The hi-lights of that 19-hour process include: the rush of adrenaline and excitement when the waters broke, a few hours of restless sleep before active labor, a beautiful sunny walk through the neighborhood, squeezing my husband's hand so that he could time contractions for me, deciding together when it was "real" enough to call Maria, my husband leading me around our bedroom so that I could walk slowly with my eyes closed, glimpsing St. Lukes in the distance and feeling reassured that backup is available but so grateful we didn't need it, the blissful relief of a long hot shower, eating plain noodles to rejuvenate and later throwing them up violently, feeling so humble and vulnerable and grateful for my husband's calm and acceptance as he held my hair, sleeping so deeply in between contractions, finally reaching a point where the only way to channel the energy was to squeeze my partner's hand, looking up from one of these contractions wiping sweaty hair from my face and seeing Maria's face as a constant presence.... finally choosing where and how to birth our son, the joy of hearing him scream when he was born and knowing that he is healthy, seeing my husband's tears of joy, hearing him say our son's name: Rohan.
We invited both of our mothers to come meet their grandson as he was still attached to me, and our naked, bloody sticky selves were cuddling and crying and smiling; I will never forget the look of wonder and joy on their faces. Later, the feelings of gratitude continued as Maria and Sue helped with the afterbirth, cleaned me, helped me to the shower and bathroom, and showed me how to begin the healing and bonding process. The night concluded with a family dinner downstairs, a birthday celebration with cake and champagne, and my husband and I going to sleep in our own bed in awe at the beautiful baby by our side. For months, I had rapturous vivid flashbacks of birthing our son.
We grew into parenthood, Rohan grew into a toddler, and we decided that he was so wonderful we should give him a sibling. This time, the first words my husband said regarding the pregnancy was: "let's make sure to call the midwives right away before they're booked." What a difference a birth makes! We were thrilled at the idea of planning another home birth, but had to reconsider this decision a few weeks later when an ultrasound confirmed we would be having twins.
Since 2007, there had been even more articles published regarding the safety of home birth, but still no data addressing twins. Looking through OB literature as well, there are very few prospective trials to prove the necessity or benefit of typical OB management of twins. The only common theme shared between OB and midwife literature is that twin births involve more risk. If I were to fight for home birth again, it would be a decision based purely on philosophy and faith. In contrast to my first uncomplicated pregnancy, I knew I could not defend my choice if a tragedy occurred delivering twins at home. Fortunately, thanks to the experience afforded by Maria and Sue, we felt stronger and more confident about navigating the hospital experience for our second delivery.
However, we noticed immediately upon starting our prenatal care that there were now many aspects of the OB style of care which we found strange and confusing. We missed those hour-long appointments! Because I was carrying twins, I was allotted a whole 20 minutes to see my provider, rather than the standard 10. We had so many questions about twins and hospital births - even with a meticulously prepared written list, there wasn't time to get clear answers on what to expect. I was asked to plan on having an epidural, so that I would be made more compliant in case of an internal version or breech extraction of twin B. I was told that even a vaginal delivery would take place in the OR, "just in case." I was told that labor should be induced if I went past 38 weeks gestation. Nearly continuous electronic fetal monitoring was planned, and it wasn't clear whether the equipment would be wireless to allow movement. Our contact with the OB was limited to efficient question-answer dialog, planning the next appointments, and doing the routine physical exams. Other than the rigid kick counts and braxton-hicks recording I was supposed to be doing twice a day, there was no energy spent encouraging me to communicate with the lives growing inside me. Adding to our anxiety was the uncertainty regarding how many support people (zero, one or two?) would be allowed in the OR for delivery; it all depended on the hospital staff on duty when I presented in labor.
Fortunately, Maria and Sue had awakened and nurtured in me an innate trust of my body and my babies. In this pregnancy, I KNEW my babies from the first trimester, and I knew they needed me to take it easy in this pregnancy. I nourished our bodies, rested, and tried to stay calm. I did my own research regarding the recommended interventions, and came to have confidence in my decision to NOT induce labor if I went past 38 weeks, and not to have an epidural "just in case." I bonded with my babies, and grew to understand which was more mellow and which more feisty, which one might have more trouble keeping food down, which one was likely to emerge first, and what position they wanted to be in. Noah (the mellow one) was breech until about 32 weeks. I sensed he was ready to turn, engaged some of the postures Maria had suggested, and he turned vertex less than 48 hours later. I knew waking up in the morning that he was now in his birthing position, though it took my OB, NST nurses and radiology techs several more weeks to believe me. Although the radiologists couldn't tell which baby would be delivered first, I sensed that Shaan would probably edge his way past Noah; he proved me right at our last ultrasound one day before their birth.
We made it just past 36 weeks when Shaan's water broke around 1:30 AM. I still harbored some anxiety about having to defend my birth plan, and was afraid of the fetal monitoring. Although I thought it would be best to tackle these hurdles before labor became too intense, I started to procrastinate. My husband and I spent some time deciding who to call and in what order, we had a final fun debate about naming the twins, we did email and Facebook. I slowly packed my backpack with a million battery powered devices for labor music and ignored my contractions. My parents arrived, and watched while I finished a bowl of cereal and meticulously peeled and ate an orange. We left home at 4 AM for the short drive. In the car, we noticed contractions were about 2-3 minutes apart, but I rationalized that was due to potholes. We breezed into L&D as a family, husband, mom and dad; I told the triage nurse my pain was a "4" (laughing to myself, 'whatever that means') and settled in with my iPod and three straps on my abdomen. She took her time trying to get the prescribed amount of fetal heart rate tracings, which took over an hour. Curtains were drawn around me as the nurse worked to admit another woman who was much more vocal in her labor than I. Meanwhile, labor was feeling more intense, but I continued to rationalize: maybe I was having trouble catching the endorphin wave because of the hospital environment? Surely the straps on my abdomen are making it more painful? Labor couldn't possibly be finishing this quickly, right? In any case, I had disappeared to that magical place within myself, and did not have the energy or will to express these thoughts to strangers.
When I was officially admitted over an hour after arrival, I was asked if I wanted to walk to the labor room or go by wheelchair. Naturally, I walked. With a chucks pad awkwardly held between my legs, three straps on my abdomen, a ridiculous hospital gown, two blankets shrouding my naked backside and three cables looped over my shoulders, I made the short journey in a daze, indulging in some feelings of martyrdom. No one had yet checked my cervix, and the triage nurse had no clue that delivery was imminent; she settled us into the room and left us, promising the doctor would be in soon. Within moments, that familiar involuntary spasm took hold, and Shaan started his descent. Because I was still standing over linoleum, my mom got in position to catch him, and my husband started hitting the red panic button and calling for a doctor. The attending OB arrived as Shaan was crowning; Shaan eased into the world with one more contraction, immediately pink and vigorous. Only a little over four hours had passed since his water had spilled forth. The pediatric team wasn't there yet, so I got several minutes to kiss his sticky head and cuddle him while the doctors worked around his cord to check Noah's position and heartbeat.
The attending doctor that evening - whom I was prepared to encounter as an adversary - turned out to be magnificent. She sized up my personality and the situation within moments, and orchestrated the atmosphere and pace of the remaining delivery beautifully. Someone mentioned if we should still move to the OR for delivery of the second baby, but she saw my face and quickly abandoned the standard protocol. No one breathed a word about epidural or IV access. This was lucky, because things really slowed down, and I'm not everyone would have had the patience or confidence to wait for Noah's birth if I were in an OR. Either due to a half-empty uterus, the joy of holding Shaan, or 8-10 strangers staring at me expectantly, I stopped having regular or meaningful contractions. Noah was still in cephalic presentation, his heartbeat was strong, and I wasn't bleeding heavily, but labor was arrested. The OB was very reassuring, but refused to leave my side - she mandated quiet calm focus. Though she didn't mention it, we all knew there was a small chance of catastrophic placental abruption or cord prolapse for Noah, whose water bag was still intact. I tried standing, moving my hips, closing my eyes, willing contractions to come, alternately relaxing and pushing, for over an hour. Pushing without the urge is somewhat like trying to sneeze at will: it's never quite as effective. Finally, the OB gently offered to do an exam to determine if it may be safe to artificially rupture Noah's bag of waters. By this time, I was quite ready to meet my third child, and gratefully accepted. Once Noah's head was better engaged, my awkward forced pushing was much more effective, and he was born about 90 minutes after Shaan. Turns out Noah had the umbilical cord tightly wound twice around his right foot - the length of cord remaining for delivery was short, which may have slowed his birth. Noah came to us in three big chunks rather than one whoosh. He was placed on my chest immediately, and I only noticed later in the pictures that his cord had been clamped against my wishes -- one small sacrifice for an otherwise perfect birth.
The attending OB asked me not to share her name, lest other women come clamoring for the OB who is supportive of an epidural-free, OR-free natural vaginal delivery of twins. But it is possible, and it was wonderful. In fact, all the doctors involved later confessed that they felt lucky to be working when my "precipitous" delivery (never mind the hour-long wait in triage) voided all protocol, so that they could witness and learn from a natural birth. Our story was shared among the staff, and we later heard from doctors on shift before and after that they were disappointed that they missed out. Perhaps most OBs in their hearts actually want to practice natural hands-on medicine, but feel bound by institutional practices and professional guidelines designed to defend against litigation. Maybe we should look into their eyes to see what they really believe when they tell us that an intervention is "recommended."
My husband and I spoke about this afterwards. The big bad hospital turned out to be full of well-meaning people who were consistently kind. The shift changes were actually nice, because each new nurse brought with her a new perspective or tip for breastfeeding or recovery. At times their insistence on frequent feedings and vital sign checks on our sleepy newborns could have undermined our confidence, but we were basking in happiness at having two healthy babies, and trusted from our first delivery that all would be well. Having twins, we were grateful for some of the efficiencies of the hospital, getting the birth certificates, social security cards, hearing screen, newborn screen, etc all done in one location. But we left exhausted from all the hospital activity, and feeling that we shared this experience more with strangers than each other. The magic of home birth was lost, and there have been no euphoric flashbacks for me. We are happy that we made the right decision for our family, grateful that we entered the hospital armed with the calm confidence instilled by our midwives, and thrilled with the outcome. But there is no place like home.

Sunday, April 4, 2010
50 Best!
Subscribe to:
Comments (Atom)